Selecting the Right Treatment
Fibroids can be treated in many ways. The treatment you choose should be based on the severity of your symptoms, your goal and your stage of life. You may not want to become pregnant, for example, but it may be important to you to avoid the complications that a hysterectomy may cause.
Your physician should conduct any one of a number of imaging tests to determine how large your fibroids are, how many you have and where they are located to see what treatment is best for you.
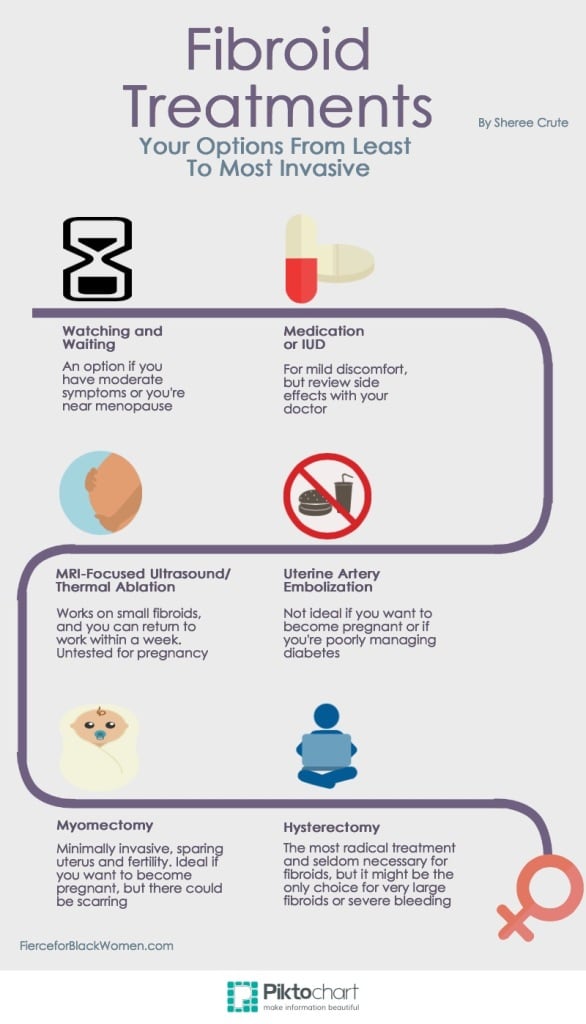
This list progresses from least invasive to most invasive treatment.
- Watching and waiting. Most women who have fibroids do not need surgery.One study focused on women whose fibroids had increased the size of their uterus to that of about a two-month pregnancy. It found that 77 percent of them chose watchful waiting and that they experienced no increase in symptoms after a year.
“There’s some evidence that eating a healthy diet and exercise can reduce tumor growth as well, but you should have regular gynecological exams,” Howell says.
Is it right for you? This is the best choice for women who have moderate symptoms or may be near menopause. After your periods stop, even the most severe fibroids will shrink and stop bleeding.
- Medication. Women with mild discomfort can take over-the-counter pain medications like ibuprofen, but you might consider several other drugs. Some work by reducing the amount of estrogen in your body; others attack inflammation. Your doctor might also suggest an IUD. The latest treatment is “the non-hormonal drug Lysteda [tranexamic acid tablets],” which reduces heavy bleeding, Bradley says.
Is it right for you? All of the medications and IUDs have side effects and may cause complications, so review each one carefully with your doctor before selecting this type of treatment.
- MRI-guided focused ultrasound or radiofrequency volumetric thermal ablation. These similar procedures do not involve surgery. A doctor uses magnetic resonance imaging to look inside the uterus and identify the fibroids. The ultrasound waves heat and destroy the fibroids, while sparing healthy tissue.
To “ablate” means to remove or destroy. When it comes to fibroids, this can be accomplished by using microwaves or electric current. The company Halt Medical has patented the Food and Drug Administration–approved Acessa System for this procedure. It effectively kills the fibroids, but there is an 11-percent reoccurrence rate.
Is it right for you? “Acessa allows you to treat small fibroids and the patient can be back to work in three to seven days,” says Jay M. Berman, M.D., chief investigator for the Acessa clinical trial. “But Acessa has not been evaluated for pregnancy, though a small number of women have become pregnant after the procedure.” (It is not known why this and other fibroid procedures might make getting pregnant or pregnancy difficult.)
- Uterine artery embolization (UAE). This is also a non-surgical procedure. UAE works by cutting off the blood supply to fibroids so that they shrink and die. A radiologist identifies the arteries with an X-ray. Using a video screen, he or she injects small particles into the uterine artery feeding the fibroid to cut off blood flow.
Is it right for you? UAE can be used to treat larger fibroids than ultrasound or ablation procedures, but it’s a poor choice if you want to become pregnant. It can cause pregnancy complications, and there’s a risk of damaging arteries to other parts of the body. It’s a particularly bad choice for women with badly managed diabetes.
- Myomectomy (open or closed). This uterus and fertility-sparing surgery involves cutting up the fibroids and removing them through a tiny incision during a closed myomectomy, which is a minimally invasive procedure. In fact, closed myomectomy has been the subject of controversy lately, but it is possible to have a safe one. (See “Fibroid Surgery Will Not Give You Cancer,” below.)
Is it right for you? “Myomectomy is the only fibroid surgery that is optimal for women who want to become pregnant,” Howell says. Whether you have minimally invasive or open surgery, a recent study found that “neither the size or the number of fibroids” should be a barrier to becoming pregnant after the procedure,” though some scarring may occur.
- Hysterectomy. The most radical of all fibroid treatment choices, hysterectomy can involve the removal of the uterus or removal of the uterus along with the fallopian tubes, cervix and ovaries. The more radical procedure causes menopause and is seldom necessary for women with fibroids.
The best way to avoid a hysterectomy is to seek fibroid treatment early, seek treatment at a fibroid center that specializes in less radical treatments and select a surgeon who is highly skilled at myomectomy and other options.
Is it right for you? Hysterectomy will end your menstrual cycle and, of course, fertility — and depending on how extensive a procedure you have, it will throw you into menopause. But it may be the only choice if you have severe bleeding or large fibroids. Hysterectomies may also cause health problems as you age, including pelvic organ prolapse, urinary incontinence and bowel dysfunction. The jury is still out on whether the surgery causes sexual dysfunction. The frank forum on the site, HysterSisters, offers helpful information on that topic.
No matter what treatment you choose, the most important thing to remember is that when it comes to fibroids, you can find the help you need. “I was so fortunate,” Thompson says. “The people around me, including the right physician, helped me to not give up.”
Sheree Crute is co-founder and editor-in-chief of FierceforBlackWomen.com. This three-part series is part of Living Well: Fierce Reports on Black Women’s Health. Part 1 focused on how your body creates fibroids. Share your story in the comments section below, and lookout for Fierce conversations on fibroids.